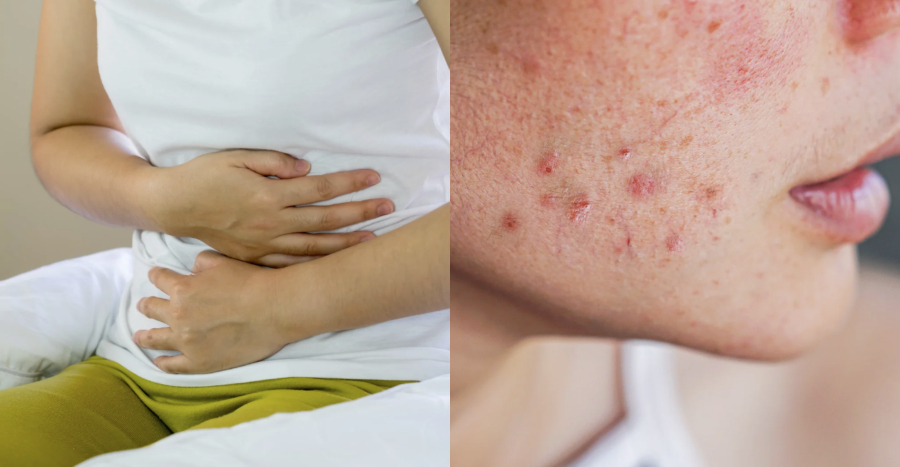
When you think of food poisoning, your mind likely conjures up images of stomach cramps, nausea, and an endless parade to the bathroom – not a sudden breakout or skin inflammation.
Yet, for some, the aftermath of food poisoning isn’t just gastrointestinal distress, but also unwelcome surprises on their skin.
How exactly does food poisoning connect to your complexion? Let’s dive into the science of the gut-skin axis and what experts say about this under-the-radar relationship.
Meet the Experts
- Dr Ang Sue May is a Consultant Dermatologist at Skincodes Dermatology. Trained in the UK, she is a registered skin specialist in both Singapore and the United Kingdom. Her areas of expertise include acne and scarring, skin cancer, and dermatological surgery.
- Dr Calvin Koh is a gastroenterologist at Mount Elizabeth Novena Hospital, Gleneagles Hospital, and Parkway East Hospital. His clinical interests lie in pancreatobiliary diseases, gastric cancer, colon cancer, and general gastroenterology and hepatology.
How Your Gut Impacts Your Skin

The connection between your gut and your skin isn’t just wellness marketing fluff – it’s science.
Dr Calvin Koh explains that gastrointestinal infections, including those caused by food poisoning, can disrupt the gut microbiota, which plays a significant role in skin health.
“Gastrointestinal infections and the medications used to treat them, like antibiotics, can cause disruptions in the healthy gut flora and contribute to worsening acne conditions,” he notes.
Stress from food poisoning, which elevates cortisol levels, further complicates the issue. Elevated cortisol can stimulate oil production in the skin, a direct trigger for acne.
Similarly, Dr Ang Sue May highlights the systemic inflammation triggered by food poisoning.
“Food poisoning disrupts the gut lining and potentially increases intestinal permeability – often referred to as ‘leaky gut.’ This allows toxins and bacteria to enter the bloodstream, triggering systemic inflammation that may manifest in the skin,” she says.
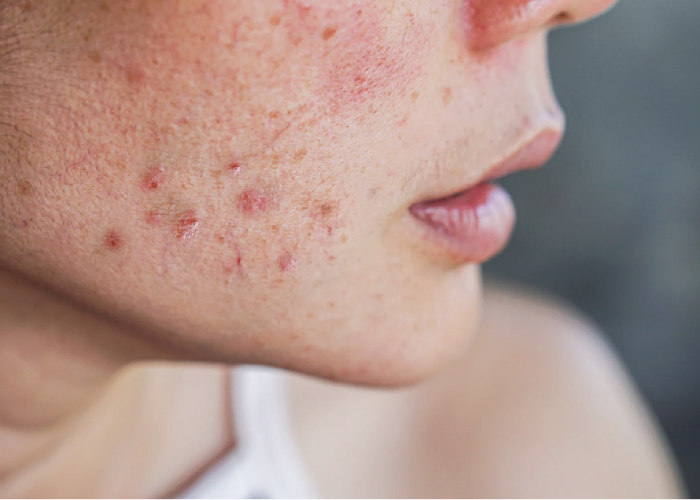
Research from the Taiwanese National Health Insurance Database, highlighted by Dr Koh, underscores this gut-skin connection.
“Although seemingly unrelated, there is some association between gastrointestinal illness and acne,” he explains.
“A study showed that patients with acne were more likely to have gastrointestinal complaints, including peptic ulcers, irritable bowel syndrome, gastroenteritis, gastroesophageal reflux disease, and constipation.”
The underlying link often involves the gut microbiota, the diverse community of bacteria in your digestive system that plays a vital role in overall health.
Studies suggest that the balance of these bacteria is often disrupted in individuals with acne. Food poisoning, with its accompanying gastrointestinal distress and potential antibiotic use, can further upset this delicate microbial ecosystem.
Ultimately, when your gut health suffers, your skin often follows suit.
Signs Your Skin Might Be Suffering Post-Food Poisoning
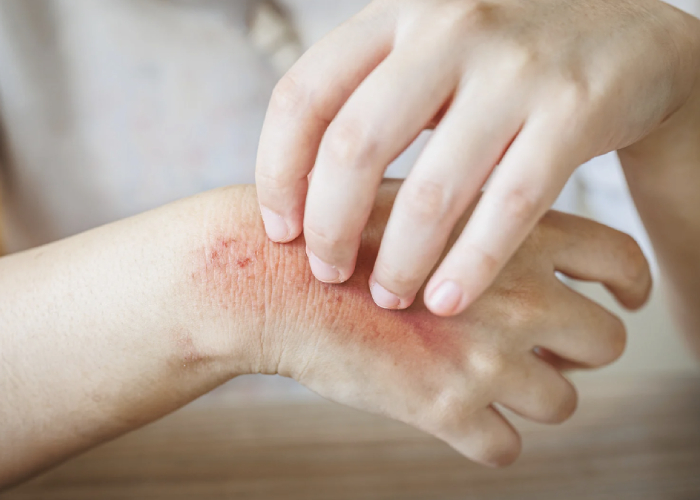
Skin issues that arise after food poisoning can vary, but inflammation is the common thread. According to Dr Ang, you might notice:
- Redness and flushing: Inflammatory cytokines released during immune responses dilate blood vessels, leading to redness or a flushed appearance.
- Breakouts: Increased sebum production and clogged pores driven by inflammation and stress hormones can worsen acne, especially in acne-prone areas like the T-zone.
- Dryness or flakiness: Dehydration caused by vomiting and diarrhoea reduces skin hydration, making it more prone to irritation.
- Hives or rash: The immune system’s response to bacterial toxins can lead to histamine release, resulting in hives or itchy welts.
Does the Type of Food Poisoning Matter?
The specific culprit behind your food poisoning might also influence skin reactions.
Dr Koh points to bacteria like E. coli, Salmonella, and Vibrio – members of the proteobacteria family – as potential triggers for systemic inflammation that can exacerbate acne. While the research is still emerging, the gut’s microbial residents appear to play a starring role in the drama.
Dehydration Sabotages Your Skin
Vomiting and diarrhoea wreak havoc on your body’s hydration levels, but the effects on your skin can be just as insidious.
Dehydrated skin struggles to maintain its barrier, leaving it vulnerable to irritants. Dr Ang warns that this can lead to overcompensating oil production, clogged pores, and increased sensitivity – setting the stage for more breakouts and irritation.
Healing Your Skin Post-Food Poisoning
Recovery starts with addressing the root cause: your gut health. Here’s what the experts recommend:
1. Support Gut Healing with Probiotics
Probiotics containing Lactobacillus acidophilus and Bifidobacterium lactis can help restore microbial balance. Dr Ang adds that these can also reduce inflammation and stabilise cortisol, minimising acne triggers.
“Probiotics also promote the production of short-chain fatty acids (like butyrate) that support the skin’s barrier function, making it more resilient to environmental irritants and less prone to dryness and sensitivity,” she explains.
Conversely, excessive fat and sugar consumption can negatively impact your gut bacteria. “Diets high in fat and sugar and low in fibre are associated with decreased presence of groups of bacteria such as Lactobacillus and Bifidobacterium,” Dr Koh says.
2. Nourish with Skin-Loving Foods

While avoiding high glycemic-index foods (like refined carbs and sugars) is key, Dr Koh suggests incorporating fermented foods, fibre-rich vegetables, and prebiotics to support a thriving microbiome.
“A varied, healthy diet in various nuts and seeds and beans, as well as fermented foods such as unsweetened yoghurt or kefir is thought to be important in microbial diversity and promote a healthy microbiome,” he informs.
“However, as some of these foods may not be so easily digestible, it may be better to wait for full recovery from the gastrointestinal infection before attempting such a diet.”
3. Rehydrate
Combat skin dehydration with a combination of oral hydration and topical moisturisers rich in ceramides and hyaluronic acid.
When Topicals and Treatments Come to the Rescue

If your skin still feels like it’s holding a grudge after food poisoning, both at-home skincare and professional treatments can help repair the damage and restore balance. Here’s how:
At-Home Topical Treatments
Dr Ang recommends focusing on ingredients that soothe inflammation, restore hydration, and repair the skin’s natural barrier. These include:
- Panthenol (Vitamin B5): This soothing ingredient hydrates and strengthens the skin barrier, locking in moisture and calming irritation. It’s particularly helpful for inflamed or sensitive skin post-breakout.
- Niacinamide (Vitamin B3): Known for its anti-inflammatory properties, niacinamide reduces redness, regulates oil production, and enhances the skin’s resilience, making it a go-to for stressed or breakout-prone skin.
- Hyaluronic acid: To counter dehydration, hyaluronic acid draws moisture into the skin, replenishing hydration levels without clogging pores.
- Ceramide-infused moisturisers: Ceramides reinforce the skin barrier, helping it recover from dehydration and making it less prone to irritation and breakouts.
For targeted acne treatment:
- Salicylic Acid (BHA): A gentle exfoliant that penetrates pores to clear out oil and impurities, salicylic acid is ideal for unclogging pores post-breakout. Use sparingly to avoid over-drying.
- Benzoyl Peroxide: Effective for inflamed acne lesions, benzoyl peroxide kills acne-causing bacteria. Opt for low concentrations (2.5 to 5%) to minimise irritation.
- Vitamin C: For lingering post-inflammatory hyperpigmentation, a low-strength vitamin C serum can help brighten skin and fade dark spots. Avoid stronger formulations if your skin feels sensitive.
In-Office Dermatological Procedures
For those dealing with persistent breakouts or inflammation, Dr Ang also highlights several in-office treatments to accelerate recovery:
- LED Light Therapy: Blue Light targets acne-causing bacteria (Propionibacterium acnes), helping to reduce active breakouts, while Red Light soothes inflammation, promotes healing, and can improve overall skin texture.
- Hydrafacial with LED add-on: This treatment combines deep cleansing, exfoliation, and hydration with LED therapy for a one-stop solution to improve skin clarity and reduce inflammation.
- Gentle chemical peels: Low-concentration peels using alpha hydroxy acids (AHAs) like lactic or mandelic acid can gently exfoliate dead skin cells, improve texture, and fade post-acne marks without aggressive peeling.
- Microneedling with hydrating serums: Microneedling boosts collagen production and enhances the absorption of hydrating serums. It can help with post-inflammatory hyperpigmentation and improve skin resilience, though it’s best suited once active inflammation subsides.
- Corticosteroid injections: For large, painful cysts or nodules, a dermatologist can administer a low-dose corticosteroid injection to reduce inflammation rapidly. This treatment not only speeds up healing but also minimises the risk of scarring.
How Long Until Your Skin Recovers?
The timeline varies. Dr Ang estimates that mild breakouts or redness might resolve in one to two weeks, but more severe inflammation could take several weeks or longer. Probiotics and consistent hydration can cut recovery time significantly, so don’t skip these essential steps.
With the right combination of at-home treatments and professional care, your skin can bounce back faster, leaving you feeling confident and clear-faced again.
Dr Ang shares some helpful tips to speed up skin recovery.
- Go easy on exfoliation: “Keep exfoliation to a minimum, especially if the skin is recovering from inflammation. Over-exfoliating can compromise the skin barrier further.”
- Patch-test new products: “Since the skin may be more sensitive, patch-test any new products on a small area first to ensure no adverse reactions.”
- Be consistent: “Consistent use of hydrating and calming products will often yield the best results without overwhelming the skin.”
Food poisoning may feel like a temporary ordeal, but its effects can linger in unexpected ways. By understanding the gut-skin connection and taking proactive steps, you can not only recover from the inside out but also protect your complexion for the long haul.
For those prone to acne or inflammatory skin conditions, food poisoning might just be another chapter in the ongoing saga of managing skin health – but armed with the right knowledge, it doesn’t have to be a permanent setback.